Diabetes Reversal: Is It a Myth or a Reality?
- devgan55
- Nov 14, 2024
- 4 min read

Type 2 diabetes has long been considered a progressive, chronic condition that can only be managed rather than cured. However, recent research and clinical observations have brought the possibility of diabetes reversal into the spotlight, raising a critical question: Is diabetes reversal a myth, or can it truly be achieved? In this article, we’ll explore what diabetes reversal really means, the current scientific understanding, and practical insights into the strategies that have shown promise.
Understanding Type 2 Diabetes and Its Roots
Type 2 diabetes is characterized by insulin resistance and elevated blood sugar levels, resulting from a combination of genetic predisposition, lifestyle factors, and metabolic imbalances. It is often driven by:
Excess body fat, particularly around the abdominal area
Poor dietary habits
Physical inactivity
Chronic inflammation
Hormonal imbalances
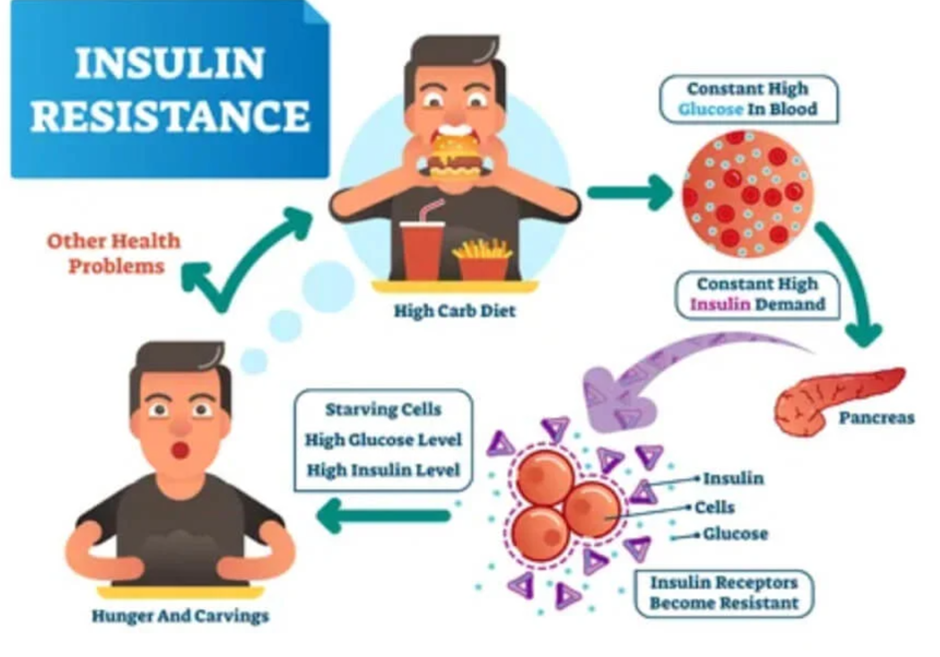
Over time, these factors lead to the pancreas producing less insulin or the body becoming less responsive to it, making blood sugar regulation increasingly difficult.
The term “diabetes reversal” generally refers to the idea that blood sugar levels can be normalized without the need for medication, achieving a non-diabetic state where the risk of diabetic complications is significantly reduced.
Diabetes Reversal vs. Remission: What’s the Difference?

Before diving into the possibilities, it’s important to define what is meant by “reversal.” Experts commonly differentiate between:
Diabetes Reversal: Achieving a state where blood glucose levels are normal without the need for diabetes medications. However, the term is not always embraced in the medical community, as the underlying causes of diabetes may remain.
Diabetes Remission: Sustained blood glucose levels below the diabetic range, often for a period of months or years, without active pharmacological treatment. Remission can be partial or full but does not necessarily mean a permanent “cure.”
Can Type 2 Diabetes Be Reversed?

While type 2 diabetes cannot be completely cured in a traditional sense, evidence shows that it can be managed to the point where symptoms are no longer present. Studies indicate that certain lifestyle interventions and dietary strategies can help some individuals achieve and maintain normal blood sugar levels. Let’s explore some of the factors associated with diabetes reversal.
1. Weight Loss, Especially Visceral Fat Loss
Substantial weight loss, particularly loss of abdominal fat, is one of the most critical factors in achieving diabetes remission. Several studies suggest that a 10-15% reduction in body weight can significantly improve insulin sensitivity and pancreatic function. One landmark study, the DiRECT Trial (Diabetes Remission Clinical Trial), showed that nearly 46% of participants who lost substantial weight maintained remission of diabetes for at least two years.
2. Low-Calorie and Very Low-Calorie Diets (VLCDs)
Research shows that significant caloric restriction can help individuals lower blood sugar levels, often to a non-diabetic range. Low-calorie diets (800–1,200 calories per day) and even very low-calorie diets (400–800 calories per day) have been effective in rapidly reducing blood glucose and improving insulin sensitivity. VLCDs are typically short-term interventions and should only be conducted under medical supervision due to the risk of nutritional deficiencies.
3. Low-Carbohydrate and Ketogenic Diets
Low-carbohydrate and ketogenic diets (keto diets) reduce the amount of glucose available in the bloodstream, allowing insulin levels to stabilize. These diets can also enhance insulin sensitivity and decrease insulin resistance over time. For some individuals, following a strict low-carb or keto diet has resulted in sustained remission of diabetes, though it may be challenging to maintain in the long term.
4. Exercise and Physical Activity
Physical activity plays a crucial role in improving insulin sensitivity and reducing body fat. Both aerobic and resistance exercise can help reduce insulin resistance, improve glucose uptake, and support overall metabolic health. Incorporating regular physical activity, especially after meals, can have a substantial impact on blood sugar control.
5. Intermittent Fasting
Intermittent fasting (IF) has emerged as a promising strategy for improving insulin sensitivity and blood sugar control. Several studies indicate that time-restricted eating, particularly when meals are consumed within an 8-10 hour window, can help regulate blood sugar levels and support metabolic health. For some, IF can help achieve sustained glycemic control and potentially aid in diabetes remission.
6. Personalized Nutrition and Medical Supervision
The response to dietary interventions varies from person to person, and individual factors such as age, genetics, and overall health can influence outcomes. Personalized nutrition guided by healthcare professionals, such as endocrinologists, nutritionists, and diabetes educators, is essential in creating sustainable, effective approaches.
Key Factors Affecting the Potential for Diabetes Reversal

1. Duration of Diabetes: The longer a person has had diabetes, the more difficult it may be to achieve remission, as the pancreatic beta cells responsible for insulin production can become progressively damaged over time.
2. Age and Overall Health: Younger individuals and those without significant complications or comorbidities may experience better outcomes with lifestyle interventions.
3. Commitment to Lifestyle Changes: Diabetes remission is typically achieved through significant dietary and lifestyle modifications, which can require substantial motivation and dedication.
4. Underlying Health Conditions: Individuals with thyroid disorders, polycystic ovary syndrome (PCOS), or other metabolic conditions may need tailored strategies, as these conditions can influence insulin resistance and blood sugar control.
Conclusion: Is Diabetes Reversal a Myth or Reality?

For many, diabetes reversal is not just a myth—it’s an achievable goal, particularly with early diagnosis and comprehensive lifestyle intervention. While the concept of a “cure” remains complex, achieving remission and living without diabetes medications is a very real possibility for some people. However, remission is often dependent on sustained lifestyle changes, and for others, maintaining tight blood sugar control may still require ongoing medication or therapeutic support.
The approach to diabetes reversal should be individualized and approached with realistic expectations. While remission is achievable, it may not be permanent, and regular monitoring, lifestyle maintenance, and possibly intermittent support are key to lasting success.

Commenti